Acinetobacter
From WikiMD's WELLNESSPEDIA
<translate>
General information about Acinetobacter[edit]
- Acinetobacter [asz−in−ée−toe–back−ter] is a group of bacteria commonly found in soil and water.
- While there are many types or “species” of Acinetobacter and all can cause human disease, Acinetobacter baumannii [asz−in−ée−toe–back−ter boe-maa-nee-ie] accounts for about 80% of reported infections.
- Outbreaks of Acinetobacter infections typically occur in intensive care units and healthcare settings housing very ill patients. Acinetobacter infections rarely occur outside of healthcare settings.
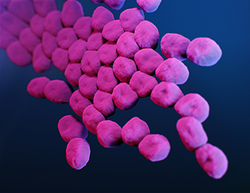
Acinetobacter
Symptoms of Acinetobacter infection[edit]
- Acinetobacter causes a variety of diseases, ranging from pneumonia to serious blood or wound infections, and the symptoms vary depending on the disease.
- Acinetobacter may also “colonize” or live in a patient without causing infection or symptoms, especially in tracheostomy sites or open wounds.
For more images of this bacterium, search the Public Health Image Library
Transmission of Acinetobacter infection[edit]
- Acinetobacter poses very little risk to healthy people.
- Acinetobacter can be spread to susceptible persons by person-to-person contact or contact with contaminated surfaces.
Immune system compromise[edit]
- People who have weakened immune systems, chronic lung disease, or diabetes may be more susceptible to infections with Acinetobacter.
- Hospitalized patients, especially very ill patients on a ventilator, those with a prolonged hospital stay, those who have open wounds, or any person with invasive devices like urinary catheters are also at greater risk for Acinetobacter infection.
Prevention of Acinetobacter infection[edit]
- Acinetobacter can live on the skin and may survive in the environment for several days.
- Careful attention to infection control procedures, such as hand hygiene and environmental cleaning, can reduce the risk of transmission.
Treatment of Acinetobacter infection[edit]
- Acinetobacter is often resistant to many commonly prescribed antibiotics.
- Acinetobacter infection typically occurs in ill patients and can either cause or contribute to death in these patients.
- Acinetobacter infections are generally treated with antibiotics.
Culture and sensitivity[edit]
- Culture and sensitivity is done to determine which are active against the germ.
- The provider will then select an antibiotic based on the activity of the antibiotic and other factors, like potential side effects or interactions with other drugs.
Antibiotic resistance[edit]
Unfortunately, many Acinetobacter germs are resistant to many antibiotics, including carbapenems, which makes them difficult to treat with available antibiotics. A-Z index of infectious diseases | Glossary of infection control | Glossary of vaccines
| Infectious disease and microbiology | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
</translate>